Coronary angiography and pci
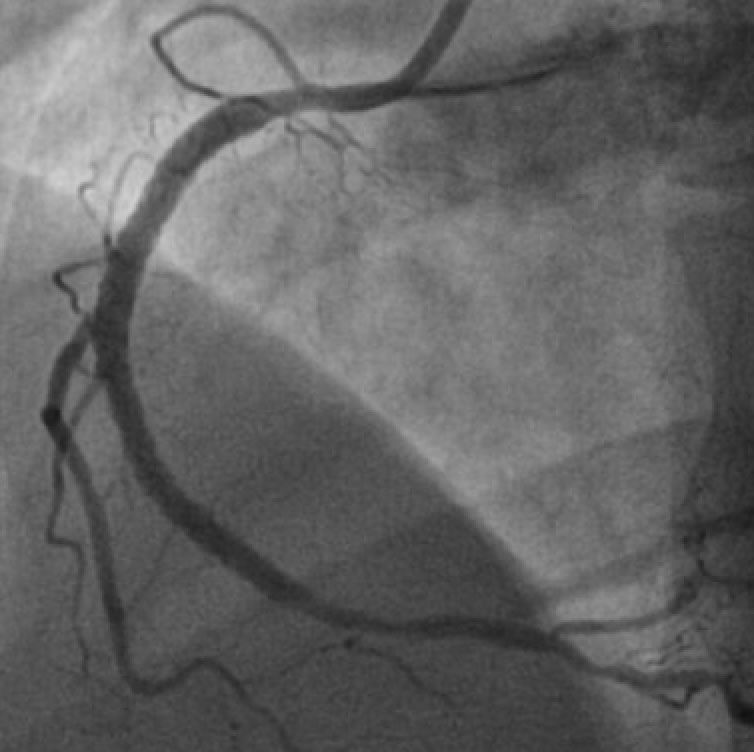
Coronary angiography with PCI is a medical procedure used to diagnose and treat coronary artery disease, a condition in which the arteries that supply blood to the heart become narrowed or blocked.
During the procedure, a thin, flexible tube called a catheter is inserted into a blood vessel, typically in the groin or arm, and advanced to the heart. A contrast dye is then injected through the catheter and into the coronary arteries, allowing them to be visualized on x-ray images.
Based on the results of the angiography, the cardiologist may recommend a percutaneous coronary intervention (PCI) to improve blood flow to the heart. PCI involves the use of a stent, which is a small metal mesh tube that is inserted into the coronary artery to keep it open and improve blood flow. There are several different types of stents available, including drug-eluting stents which release medication to prevent the artery from becoming blocked again.
During the PCI procedure, the cardiologist uses imaging technology, such as intravascular ultrasound (IVUS) or optical coherence tomography (OCT), to guide the stent placement. IVUS uses sound waves to create detailed images of the coronary arteries, while OCT uses light waves to create high-resolution images. These technologies allow the cardiologist to accurately place the stent in the optimal location within the coronary artery.
PCI with coronary angiography is a safe and effective procedure for treating coronary artery disease. It has been shown to reduce the risk of heart attack, improve symptoms, and improve quality of life. However, as with any medical procedure, there are potential risks and complications, including bleeding, infection, and damage to the blood vessels or heart. It is important to discuss the benefits and risks of coronary angiography with PCI with your cardiologist to determine if the procedure is right for you.